Yusuf Ransome, Ph.D., assistant professor in the Department of Social and Behavioral Sciences at the Yale School of Public Health, researches HIV/AIDS. He studies how social, economic and cultural determinants influence racial/ethnic- and geography-related disparities in the HIV care continuum using factors such as social capital and religion, faith and spirituality.
To identify and understand these complex trends, he uses survey data analysis, multilevel modeling, structural equation modeling, spatial epidemiology and geographic information systems. On today, World AIDS Day, Ransome takes some time to discuss the challenges ahead in the HIV/AIDS epidemic and what needs to be done to reduce and eliminate disparities.
Racial disparities in HIV incidence in the United States have persisted for decades, even after the introduction of PrEP. Will racial disparities in HIV persist in the decades ahead?
YR: In 2010, the estimated HIV incidence was 55 vs 6 per 100,000 persons (chart), 9-times higher for Blacks than Whites, respectively, and those disparities remained in 2019 (estimated incidence 8.4 times higher). As we mark 40 years of HIV/AIDS we need to learn from the past and adopt radical approaches to eliminate disparities. There is an urgency for culturally responsive interventions that, at the core, are rooted in sociocultural factors such as social norms, religion and spirituality, and social connectedness, and social capital within communities of color. 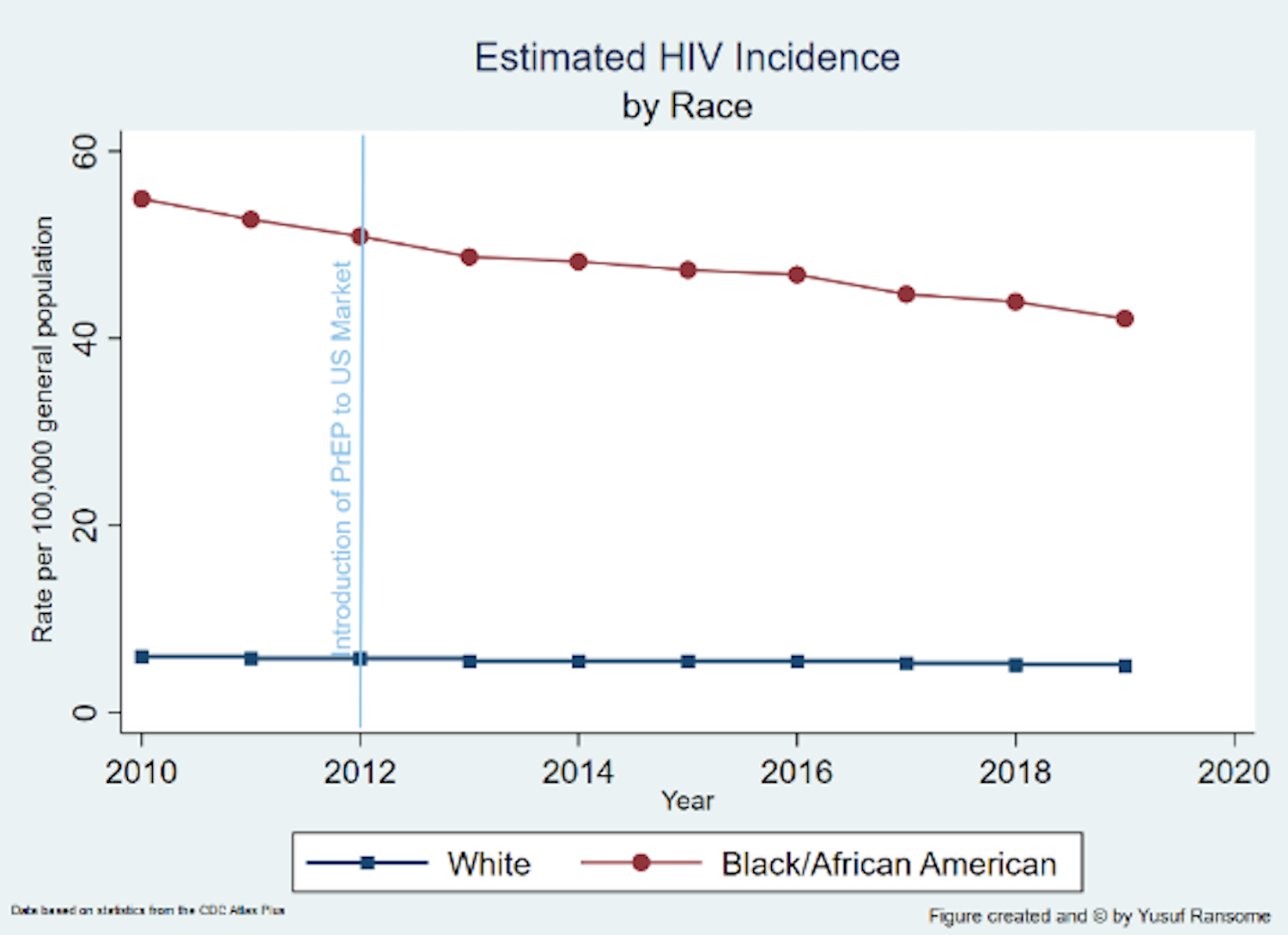
Social determinants of health were major risk factors that resulted in disparities in COVID-19 infections. Several of those factors (e.g., employment and access to care) are also associated with higher HIV risk. Will this recognition help improve interventions that contribute to greater equity in HIV-related outcomes?
YR: Socioeconomic conditions were risk factors for crack/cocaine use that drove the spread of HIV among African Americans in the 1980s. The subsequent decades of social, fiscal and (in)justice policies that followed (and failed) (e.g., the War on Drugs) underscored the need for society to address substance misuse as a public health problem. Addressing socioeconomic risk factors of substance misuse is beneficial for everyone because no social group was immune from the health consequences of a fragmented approach to opioid and HIV risk. With the COVID-19 pandemic, the same is true. Socioeconomic determinants (e.g., likelihood of being a frontline worker or the inability to work from home) are greater risk factors for COVID-19 exposure and infection for Black/African Americans, immigrants and low-income individuals. Yet, not addressing these issues among those groups will continue to affect ALL Americans. We cannot treat this problem without an equity lens because it is everyone’s problem. As we turn the tide in the COVID-19 pandemic, HIV is still here. We can learn from these epidemics to invigorate our approaches to HIV prevention. Equitable outcomes will depend on how the legislative and business sectors create, target and market interventions to address both COVID-19 and HIV risk.
There is an unprecedented array of biomedical technologies to test for COVID-19, treat COVID-19 infections, and mitigate COVID-19 infection risk. Will this arsenal of technology contribute to reducing new HIV infection?
YR: More technology is good but insufficient unless we address the psychosocial aspects of prevention. We need an equity-centered approach that explicitly acknowledges that infectious diseases like COVID-19 and HIV often do not occur in isolation. Design thinking and technologies thus, should be multi-focused and deployed to achieve multiple outcomes (e.g., bio-social-behavioral interventions that offer COVID-19 and HIV rapid testing capabilities together). Beyond the potential future of COVID-19 and HIV-related technology, we must address the psychosocial issues related to technology. “The Jab” is a frequent term used for receiving the COVID-19 vaccine, yet, that term often connotes something negative. Once etched in the psyche of individuals, when COVID-19 is over (and the threat of HIV remains) what are our expectations for uptake of HIV biomedical technologies like long-acting injectable PrEP? We have made significant and lightening speed advancements in technology to stem COVID-19, and we should be proud. Yet, we must keep one eye on the prize of eliminating HIV, and the key will be equity-design thinking that maximizes the utility of technologies to address disease syndemics.
3 Essential Questions (3EQ) is a recurring feature that explores vital topics in public health. Read earlier versions of 3EQ on cancer, antibiotic resistance, climate change and recreational marijuana.
MEDIA CONTACT:
Michael Greenwood at Michael.greenwood@yale.edu
Credit: Source link


